Many air medical programs face a dilemma when it comes to sharing aviation knowledge with medical crews: how much is too much?
Educating nurses and paramedics about topics like weather, navigation, and aircraft systems can make them more valuable partners in crew resource management. But some pilots worry that such training only leads clinicians to doubt their pilots’ judgment, encouraging them to interfere in matters they don’t fully understand. Their concern reflects a fundamental distrust between medical crewmembers and the people who fly them, with crewmembers too often suspecting that their pilots are trying to kill them, and pilots suspecting that their crewmembers are trying to get them fired.
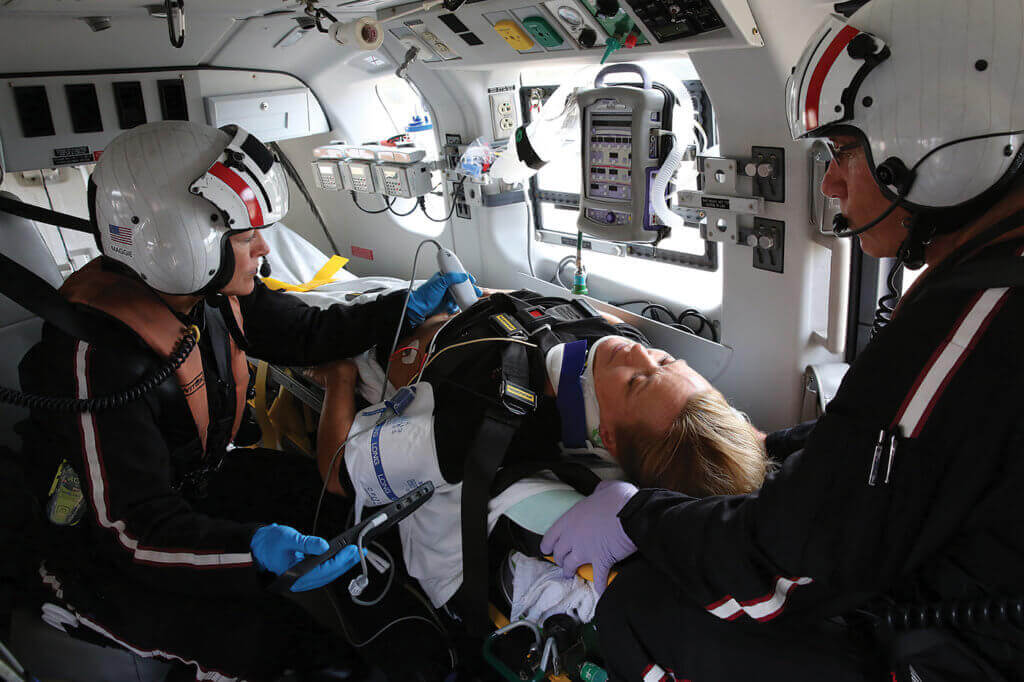
For Sentara Healthcare’s Nightingale Regional Air Ambulance program, based in Norfolk, Virginia, this dilemma simply doesn’t exist. Nightingale’s position is simple: the more knowledge they can give their crewmembers, the better. And so, when new nurses and paramedics come on board, their pilots don’t simply brief them on how to open the doors and fasten their seatbelts. Instead, they lead them through a comprehensive aviation ground school, covering subjects including aerodynamics, flight physiology, weather, regulations, navigational procedures, and more.
Once that ground school is complete, new clinicians undergo an orientation period by riding along with an experienced nurse and paramedic, observing and participating in patient care while continuing to learn about the helicopter. Their education doesn’t end when this initial training is complete — aviation subjects are constantly revisited during standard crew shift change briefings and reinforced with monthly cockpit quizzes.
Flight nurse Lisa Scott recalled that when she joined the Nightingale program, “I said, ‘Wait a minute, I’m a nurse. I don’t know anything about aviation.'” But she found that the training increased her comfort level with the aircraft and her flight crews. Now, she said, “I feel that anyone who’s going to work in the machine should have some kind of knowledge about it.”

This doesn’t mean that she’s telling the pilots how to do their jobs. “We know our limits — we’re not pilots,” emphasized program manager and flight nurse Denise Baylous. Instead, Nightingale’s focus on aviation knowledge has increased the mutual respect between pilots and crewmembers, making for an effective, close-knit team that sets an example for the rest of the industry.
Serving their community
The Nightingale Regional Air Ambulance program is based at Sentara Norfolk General Hospital, located at the center of the Hampton Roads metropolitan area at the mouth of Chesapeake Bay. The area is home to Naval Station Norfolk and the Norfolk Naval Shipyard, where the U.S. Navy’s massive carrier ships and submarines are built and maintained.
Earlier this year, the Nightingale program celebrated its 35th anniversary, having performed its first flight on Feb. 25, 1982. The single-aircraft program is small, but it has made a big impact in its community, with more than 20,000 accident-free missions to its credit over the past three-and-a-half decades.
Nightingale launched its operations with a Bell 206L-1 LongRanger helicopter. In 1984, it upgraded to a twin-engine MBB Bo.105, which it refurbished in 1991. Five years later, it replaced the Bo.105 with its larger cousin, a Eurocopter (now Airbus Helicopters) BK117. Today, the program flies an Airbus EC145, which Sentara Healthcare acquired in 2011 following a two-year community fundraising campaign by the Sentara Foundation. The aircraft is operated by Metro Aviation, which also performed its completion, working closely with the Nightingale team to tailor the helicopter to their specific needs.
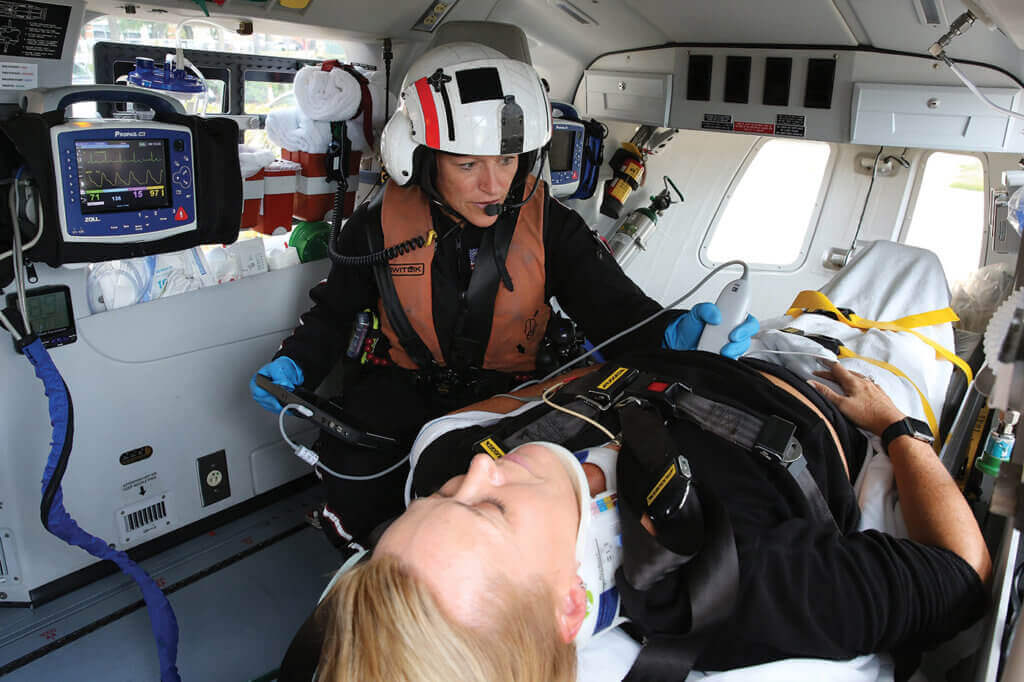
“It was fun for us to be able to sit down and do that,” Baylous recalled. The result, she said, was a carefully laid out, “fully functional critical care unit” that provides crewmembers with the space and tools they need to do their jobs. Essential medical equipment includes a CareFusion ReVel ventilator, two Zoll Propaq MD monitor/defibrillators, and three BodyGuard infusion pumps with up to six critical drips. The helicopter also carries some specialty equipment, such as a portable ultrasound machine with chest and abdominal probes, an intra-aortic balloon pump, and an IntuBrite video laryngoscope for difficult intubation cases.
The two medical crewmembers — a flight nurse and paramedic — fly with a crew iPad loaded with references, policies, and procedures; a radio frequency list; a list of all designated landing zones in their coverage area; and the Flight Vector mapping app. En route to calls, crewmembers alternate who sits up front with the pilot, giving all of them valuable experience with operating the GPS and talking to ground units on the radio. The cockpit is equipped with Garmin GNS 530 and 430 GPS units, GTX 330 transponder, GMX200 weather radar, a Technisonic TDFM-7000 transceiver, and a SkyConnect satellite phone for talk and text in emergencies. Nightingale also plans to integrate the Outerlink IRIS system for satellite tracking and flight data monitoring.
The helicopter is wired so that medical crewmembers in the left seat and the cabin can hear all terrain alerts and emergency gongs. “We wanted that,” explained pilot Jim Garrow. “We believe this is first a helicopter and second an ambulance.”
With the EC145, the program can cover a 125-mile radius without refueling, although the average flight is around 25 to 30 minutes each way. And there are a lot of flights. Last year, with just a single helicopter, the program performed more than 740 transports, of which approximately 60 percent were interfacility transports, and 40 percent scene calls.

The Nightingale program is staffed by four pilots and two mechanics employed by Metro Aviation; and six full-time nurses, 11 part-time paramedics, and six dedicated dispatchers employed by Sentara. (All of the paramedics also work on ground ambulances, which helps the program keep up rapport with local fire departments and other first responders.) Turnover in the program is low, and hiring standards are high. Paramedics who apply to Nightingale are required to have at least five years of active experience at the paramedic level in a high-volume EMS system, while flight nurses must have at least five years of critical care experience — although new hires often exceed these minimums.
Pilots, meanwhile, are required to have at least 2,000 hours of flight time, and hold a commercial pilot certificate with an instrument rating. The proximity of Naval Station Norfolk and other military installations means that military pilots are disproportionately represented in the hiring pool; of Nightingale’s current pilots, two are former Navy, one is former Coast Guard, and one is ex-Army.
That proximity to military installations means that Nightingale regularly interfaces with Navy and Coast Guard units that may have occasion to land at the Sentara Norfolk helipad. The program conducts regular training with Navy and Coast Guard crews to help ensure safe, efficient patient handoffs. When hospital construction disrupted normal operations, Nightingale brought in representatives from local air units to see the changes and discuss new procedures. The program even developed an information sheet for military pilots to keep on their kneeboards. “It’s all about breaking down silos and barriers,” said Baylous.
Sentara’s dispatch center has also integrated with Navy and Coast Guard dispatch centers — and dispatchers are as much a part of the Nightingale team as its pilots and clinicians. “I think this program has worked hard to make them part of the team,” said Lisa Scott. “We trust [them] with our safety.”

Four full-time dispatchers work three 12-and-a-half-hour shifts per week; another two dispatchers are employed on a part-time basis. “It’s a small group, so [we’ve] got to be flexible and have each other’s backs,” noted dispatcher George Pettit. Everyone who comes to work in the role has previous dispatch experience, which is critical during busy, high-stress calls. “There’s a lot for us to do in a short time if we get a flight — especially if it’s a short flight,” said Pettit.
New capabilities
According to Baylous, the Nightingale program has benefited from the unwavering support of Sentara Healthcare. Nightingale operates at a financial loss (US$1.2 million in 2014), but Sentara continues to invest in new technologies and capabilities for the program. “They see us as a community service,” Baylous explained. “They are very, very supportive in anything and all we’re doing.”
The program is now tackling a major upgrade to its capabilities by transitioning from a visual flight rules (VFR)-only program to an instrument flight rules (IFR)-capable one. Nightingale began exploring the transition once it acquired the EC145, its first IFR-certified helicopter.
Baylous said the program has taken a “crawl, walk, run” approach to adopting IFR, wanting to ensure that crewmembers fully understand and accept it. As paramedic Jeremy Miller recalled, initially “there was some hesitation” among crewmembers, just because the concept was new to them. But the Nightingale pilots’ prior military instrument flying experience provided a comfort factor. “What makes a difference is the caliber of the pilots we have here,” he said.

Sentara has been working with Hickok & Associates to develop instrument approaches for its various hospitals and freestanding helipads, aiming to have eight approaches in total. According to Jim Garrow, because winter freezing levels preclude IFR during many of the worst weather months, IFR operations will probably make up a fairly small percentage of the program’s total flights. However, having IFR capability will also allow Nightingale to perform some flights in marginal weather more safely than they could under VFR.
And safety will always remain the priority for Nightingale, which developed its innovative approach to crewmember training as a response to safety problems in the wider helicopter air ambulance industry. “I know when I first came here we weren’t as integrated as we are now,” observed Baylous, crediting former Nightingale pilot Richard Fedoriowicz with leading the initiative. By bringing crewmembers deeper into the world of aviation, “we pushed ourselves slightly outside of our comfort zones,” Baylous said. Now, however, they wouldn’t have it any other way.
Scott remarked that when she speaks with people from other helicopter air ambulance programs, she’s often surprised at the lack of interaction and partnership between medical and flight crews. Having flown with only one program, Nightingale, she only has one model for the relationship between pilots and clinicians — and it’s a positive one.
“You have to be comfortable with the person you’re working with,” she said. “You have to have that trust.”






Should I assume that the program in capable of Night Vision Goggle operations? Safety being it’s primary concern, I’m sure it was just left out by accident. Right?
Apologies for the omission. Yes, the program added NVG capabilities when it became a Metro Aviation operations customer in 2011.